More than 10% of newborn babies has a tongue band that is too short. Lip bands that are too short are slightly less common. Immediately during breastfeeding, too short bands (lip and/or tongue) often cause problems. Sometimes a baby is not even successful in drinking from a bottle. In later life, limiting bands can lead to open mouth behavior, abnormal swallowing, abnormal jaw growth, dental abnormalities, pronunciation problems, incorrect posture, snoring and sleep apnea. Oro-myofunctional therapy (OMFT) can then restore the imbalance in the functioning of the muscles in and around the mouth. This article provides information about (the consequences of) limiting bands and the treatment that the OMFT therapist can offer.
Lip tie
The upper and lower lips each have their own lip band, which ensures that the lips remain in place during all kinds of movements, such as smiling and puckering the lips. In case of a baby, a too short lip band (also called: lip tie) can cause problems during breastfeeding. The baby will not be able to curl the lips out enough to obtain a good seal around the breast. The baby regularly releases the breast and drinks restlessly. If there is a lip band that is too short, there is a very good chance that there is also a tongue band that is too short.
Tongue tie
The tongue band runs from the bottom of the tongue to the bottom of the mouth. It is tissue that starts in the front of the tip of the tongue (as growth stimulator of the tongue) during embryonic development and has to disappear slowly. If this is not done sufficiently, this is called an ankyloglossia (the Greek word ‘ankylos’ means: bound). A tongue band that is too short (also called: tongue tie) is therefore a congenital defect, whereby the tissue that connects the tongue to the mouth bottom is limiting. A tongue band may be too short, too tight, thickened and/or attached too far to the tip of the tongue. This limits the freedom of movement of the tongue. Already during pregnancy, there is a limitation of the upward movement of the tongue in the mouth, so that sometimes there is a narrow palate at birth. A tongue band that is too short is often hereditary. Usually the mother or father, or a close family member, has also suffered or suffered from it (Irene Marchesan, 2004). There are more boys than girls with a restrictive tongue band (3: 1 ratio).


Breast feeding with a lip tie
It is important to check as soon as possible after birth whether there are too short lip bands (lip tie) or a too short tongue band (tongue tie). Limitations of the bands lead almost immediately to problems. When a baby with a lip tie is breastfed, the baby may have trouble making a vacuum to the breast, causing a clacking sound when drinking. The nipple cannot be taken far enough into the mouth. Also, the baby cannot push the tongue up against the palate during drinking. The milk is held in the mouth by curling the barrel edges.
In addition to the milk, air is also swallowed (the closure of the nasopharynx is insufficient), causing colic and/or reflux. A baby’s stomach is quite high. When the baby drinks in fits and starts and also swallows air with it, it becomes restless in the stomach. This raises the milk mixed with gastric juices. This is painful for the baby.
Derived problems during breast feeding
When drinking with a restrictive tongue band and/or lip bands, the baby cannot realize sufficient suction. The incorrect way of drinking can cause blistering of the tongue and lips. Often milk production in the mother decreases, resulting in a decrease in the baby’s body weight. Because the baby has difficulty swallowing, milk residues (white deposits) are visible on the tongue. Mothers indicate that feeding takes a long time and is painful (sore nipples).
Because breastfeeding with these problems is uncomfortable for both mother and child, many mothers stop breastfeeding (decrease from 90% to 25% within six months of the birth of the baby) and switch to bottle feeding, which has a negative effect on the orofacial muscle balance in and around the mouth.
Surgial correction
A lip tie and a tongue tie can be remedied with surgical correction with scissors, laser or electrosurgery. Experience shows that a frenulectomy by laser or electrosurgery yields a good result.
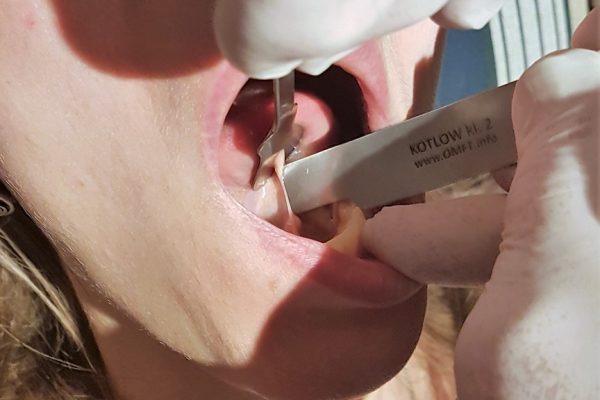
Whether a tongue band is too short can be determined from the length measurements established by pediatrician Lawrence Kotlow (the Kotlow ratings). OMFT.info has developed Kotlow rulers based on these guidelines. Useful tools to quickly and properly determine when referral for correction is sensible.
If the intervention has taken place, post-treatment by means of massage and stretching of the treated part is very important! This is to prevent relapse. After correction for babies, the lactation consultant will provide advice on after-treatment. Drinking at the breast can still be difficult after correction. This is due to the resulting compensation behavior (for example, tightening jaw clamps or shoulders). An osteopath can help in these cases.
Problems at a later age
A lip tie or tongue tie do not in all cases lead to breastfeeding problems. For example, if the mother has a perfectly shaped nipple, has sufficient nutrition and the baby’s mouth is sufficiently elastic. It is therefore the case that the bands that are too short are only discovered at a later age. Often after this has led to other problems. Because a tongue band that is too short – and the associated low tongue position – affects skeletal development and overall health. This results in an incorrect balance of the mouth and facial muscles. Possible consequences could be:
– open mouth behavior;
– mouth breathing;
– ‘flaccid’ lip tension;
– hypotonia in the face;
– an abnormal swallow;
– a narrow and high (‘Gothic’) palate;
– incorrect position of teeth, molars or jaws, such as cross bite;
– deviating pronunciation of the [l, n, d, t, t, s / z], swish or lisp;
– difficulty swallowing or eating;
– snoring;
– sleep apnea;
– a hypotonic muscle pattern and incorrect posture (hollow back and/or top of back curved);
– preposition of the head (head protrudes too far);
– a relapse after orthodontic or dental surgery treatments, because the ‘corrected’ deviation returns (partially);
– difficulties in keeping an otherwise perfectly manufactured denture in place;
– temporomandibular joint complaints.
These problems can be treated with oro-myofunctional therapy, which restores the imbalance in the functioning of the muscles in and around the mouth. The OMFT speech therapist is also the right person for after-treatment if a surgical correction of the tongue band and/or the lip bands takes place at a later age.
The treatment of (the effects of) deviating mouth orders
After the intake and the examination, it can be determined whether there are abnormal functions in the mouth area. If this is the case, oro-myofunctional therapy can start. Depending on the diagnosis and treatment goals, therapy usually consists of the following components:
• Unlearning deviant mouth behavior such as thumb and finger sucking, teat sucking and mouth breathing.
• Learning an improved tongue position at rest.
• Teaching a correct swallowing pattern.
• Optimizing the pronunciation
• Automating the new oral behavior; the new behavior must be instilled in everyday life.
When to start?
To limit the consequences of abnormal oral behavior, it is important to start treatment as early as possible. That is why younger children from the age of 3 are already referred for a preliminary phase of OMFT. This preliminary phase consists of providing parents with information about the causes and consequences of the deviant mouth habits, strengthening the mouth muscles, unlearning sucking habits and obtaining a good mouth closure.
When the actual OMFT can be started depends on the age, motivation, severity of the dental defect and the severity of the speech-language defect. OMFT focuses on children from six years and adults. The motivation for therapy should be examined per person. One child is more aware of wrong habits than the other child. One also gets treated earlier than the other.




